Radiologia Brasileira - Publicação Científica Oficial do Colégio Brasileiro de Radiologia
AMB - Associação Médica Brasileira CNA - Comissão Nacional de Acreditação
 Vol. 40 nº 1 - Jan. /Feb. of 2007
Vol. 40 nº 1 - Jan. /Feb. of 2007
|
ICONOGRAPHIC ESSAY
|
|
Sonographic findings in non-neoplastic testicular lesions |
|
|
Autho(rs): Ricardo Jorge Vital, Leandro Accardo de Mattos, Luís Ronan Marquez Ferreira de Souza, Sizenildo da Silva Figueirêdo, Jacob Szejnfeld |
|
|
Keywords: Testis, Benign testicular lesions, Ultrasonography, Color Doppler |
|
|
Abstract:
IMDs, Radiologists, Titular Members of Colégio Brasileiro de Radiologia e Diagnóstico por Imagem
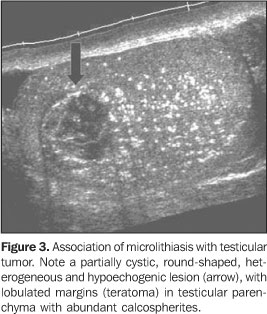
TESTICULAR MICROLITHIASIS Microlithiasis has been recently described and is a relativelyrare entity, reported to be incidentally observed in 0.6% to0.75% of patients submitted to testicularultrasound(1–4). Frequently, both testicles areaffected, however there are reports on unilaterality in patientsfrom 10 months to 70 years of age(4,5). The disease is clinically asymptomatic(2)and its cause remains unknown. The incidental diagnosis shouldindicate a complete clinical evaluation for detectingsubfertility/infertility or systemic diseases. Histologically, microliths represent scattered laminatedcalcium deposits in the lumina of the seminiferous tubules,called calcospherites(6). It may be associated with other pathological entities likeKlinefelter's syndrome, cryptorchism, Down syndrome, malepseudohermaphroditism, pulmonary alveolar microlithiasis,previous radiotherapy and infertilityconditions(7). Initially, testicular microlithiasis was thought to be a benign process not requiring follow-up(7). However, a strong association has been seen with the presence of germ cell tumors, particularly seminomas(5), and intratubular germ cell neoplasms which progress to carcinoma 50% of times (Figure 3).
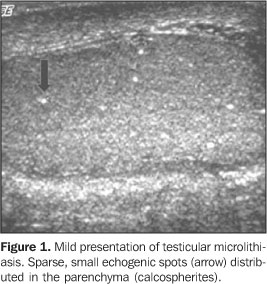
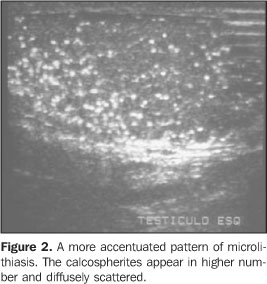
At ultrasound, the most characteristic aspect of microlithiasis is of multiple, small, hyperechogenic foci ranging between 1 mm and 3 mm in diameter, which typically do not shadow(2,8). Calcifications appear diffusely scattered throughout the testicular parenchyma, but may be segmented or distributed peripherically (Figures 1 and 2). Although not presenting posterior acoustic shadowing, occasionally they might generate comet-tail artifacts or a scintillating pattern at color Doppler(2). For the ultrasound diagnosis, the identification of a minimumof five microcalcifications per imaging field is the mostaccepted criterion(9). There are scientific evidences justifying the ultrasoundfollow-up of patients with microlithiasis, aiming at the earlydiagnosis of testicular tumors. Some authors have recommended anannual ultrasound follow-up, and that self-examination isencouraged for all patientsaffected(2,4,10).
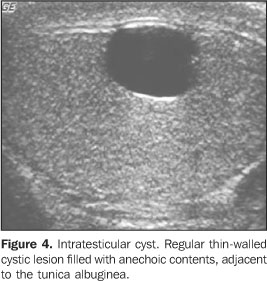
SIMPLE INTRATESTICULAR CYST Intratesticular cysts are incidentally detected lesions in menwith 40 or more years of age, measuring from 2 mm to 2 cm indiameter. They may be uni- ormultiloculated(2), usually are single andnon-palpable, and may be multiple andbilateral(11,12). The pathogenesis is still to be completely known; threetheories have been proposed: a) congenital, where simpleintratesticular cysts would be a result from an increase inepithelial cells secretion or cystic distention from remnants ofMüllerian and Wolffian ducts; b) post-traumatic; c)post-inflammatory. Microscopically, they are lined by flat or cuboid epithelium,surrounded by testicular parenchyma, with serouscontent(2). They may be found in any portion of the testes, but are morefrequently seen near the mediastinum testis and adjacent to thetunica albuginea, associated with extratesticularspermatocele. At ultrasound, the simple cyst present as an anechoic, well-defined lesion, with imperceptible walls and posterior acoustic shadowing, localized inside the testicular parenchyma(11) (Figure 4).
When complicated with hemorrhage and infection, these cystsloose their anechoic feature, and start showing internalsuspended echoes, resulting in differential diagnosis withepidermoid cyst and teratoma(2). Simple intratesticular cysts may be associated with othercongenital anomalies like Von Hippel-Lindau syndrome and cysticdysplasias(13).
INTRATESTICULAR SPERMATOCELE Spermatocele refers to an intraparenchymatous cystic lesionadjacent to the mediastinum testis, in the area of rete testis,and may be septate and communicating with seminiferoustubules. At histological evaluation, they present a fibromuscular wallsurrounded by cuboid epithelium, pseudostratified or ciliatedepithelium being rarely observed(14). Ultrasound usually demonstrates anechoic lesions measuringbetween 1 cm and 2 cm, and that may reach more than 15 cm, withposterior acoustic enhancement. Spermatoceles might be confusedwith simple cysts, although its walls use to be moreirregular(11,15,16).
INTRATESTICULAR VARICOCELE While extratesticular varicocele is a common clinicalcondition, its intratesticular form is a rare entity which isseen in less than 2% of a population affected by scrotalsymptoms(1,17). Intratesticular varicocelesusually are left-sided, in association with ipsilateralextratesticular varicoceles, but their independent existence ismore common. The most frequent claim of patients is local pain, whileinfertility, edema or scrotal mass also present as typicalsymptoms. Its sonographic appearance consists of multiple serpiginoustubular and anechoic structures, varying in sizes, usually largerthan 3 mm in diameter, localized around the mediastinumtestis(18). These vessels are more frequentlyfound at left, during Valsalva maneuver, preferably in theorthostatic position. At the mapping with color Doppler, the venous reflux is seenat the Valsalva maneuver, which ispathognomonic(1,19). The differential diagnosisincludes testicular cysts, tubular ectasia of the rete testis,hematoma, focal orchitis and cystic intratesticularneoplasms(17). There is a great controversy about which would be the mostreliable sonographic diagnostic characteristic of initial/mildvaricocele. A consensus is still to be reached about this matter,but most of urologists, in our practical experience, consider thevenous reflux as a more reliable feature than the venousdilatation.
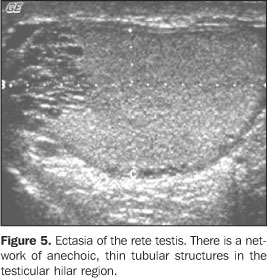
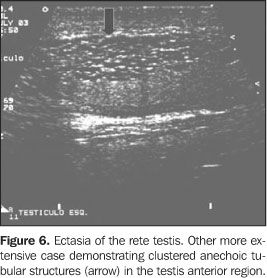
TUBULAR ECTASIA OF THE RETE TESTIS Tubular ectasia of the rete testis is a relatively rare benignentity resulting from a partial or complete obstruction ofefferent ducts(16). This obstruction may occurat different levels, and may be classified into intra- orextratesticular. In testicular lesions, the obstruction is situated in theseminiferous tubules or in the rete testis, generally resultingfrom severe inflammatory episodes like orchitis. Inextratesticular lesions, the proximal obstructions result fromluxation or traumatic tearing of epididymis, testicularvaricoceles and cystic dysplasia. Middle obstructions are due totypical epididymal conditions like epididymitis, spermatocelesand tunica albuginea cysts. On the other hand, distalobstructions occur post-vasectomy or after scrotalsurgery(8,20). Usually, these lesions affectpatients above 55 years of age, and frequently are bilateral(45%) and asymptomatic(2,21). The typical presentation of the rete testis consists of aserpiginous, hypoechoic structure communicating the mediastinumtestis with the epididymis head usually localized in theposterolateral region of the testes(20). In cases of ectasia, ultrasound depicts numerous small tubular and cystic structures with fluid and hypoechoic contents in the region of the rete testis, proximal to the mediastinum testis. At the mapping with color Doppler no flow is detected within the rete testis(16), differentiating it from the intratesticular varicoceles. Occasionally, a pseudocystic pattern may be identified(2) (Figures 5 and 6).
It is important to differentiate tubular ectasia of the retetestis from testicular tumors such as adenocarcinoma of the retetestis, epididymal cystadenoma, teratoma, non-Hodgkin lymphoma,and seminiferous tubules dilatation secondary to testicularneoplasms(16,22). In dubious cases, magnetic resonance might be of help, showingnon-enhanceable tubular structures after intravenous gadoliniuminjection, with homogeneous low-intensity signal in T1-weightedimages, and high-intensity or intermediary signal on T2-weightedimages(22).
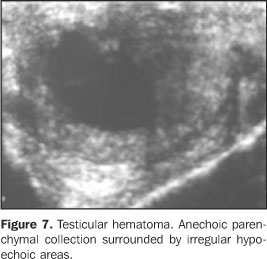
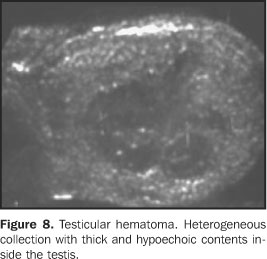
TESTICULAR TRAUMA Testicular traumas usually result from car accidents, orcontact sports, and may lead to contusion, hematoma, fracture oreven testicular rupture which is considered as a surgicalemergency(21). In closed traumas, there is aformal indication for ultrasound to evaluate the testicularviability, vascularization, and to serve as a basis forfollow-up(6). Hematomas are identified at ultrasound as heterogeneous testicular lesions, and may become complex, with cystic components. Considering the frequency of post-traumatic atrophy, the ultrasound follow-up is essential until the complete resolution of testicular alterations. This atrophy occurs as a result of ischemia caused by increased pressure inside the tunica albuginea secondary to hematoma formation(23) (Figures 7 and 8).
Tunica albuginea fracture is another condition characterizedby a fault (interruption) on the organ borders, an even externalprotrusion of the testicular pulp due to the segmentalinterruption of the echogenic testicular coat (tunicaalbuginea)(1). On the other hand the diagnosis of testicular fracture is madewhen there is a linear, irregular, hypoechoic intratesticularabnormality, dividing the testis into two or more parts. Thedifferential diagnosis with a transmediastinal artery is noteasy. Fractures with severe testicular injury present with aheterogeneous echotexture(1).
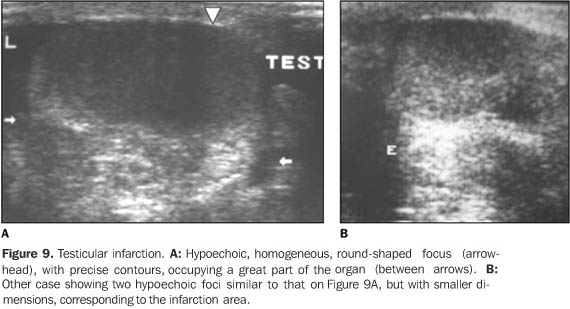
TESTICULAR INFARCTION Testicular infarction is associated with episodes of subacutetorsion or infectious phenomenon determining zones of ischemia inthe testicular parenchyma(2). More rarely,segmental infarcts are disclosed during a picture of accentuatedpain due to several etiologies such as trauma, arterial embolism,venous thromboses and various angiopathies(2).Other iatrogenic origin is the resection or connection of thespermatic cord vascular elements in an inguinal hernioplasty. Its sonographic appearance depends on the patient's age and severity of the injury(23). In an early phase, ultrasound does not demonstrate any change in echogenicity. Posteriorly, ischemic zones may be single or multiple, and appear round-shaped and hypoechoic on a plane, and in a more triangular shape with poorly defined borders on the perpendicular plane (Figure 9).
The mapping with color Doppler shows perfusion ofhypervascularized perilesional regions and/or absent flow in thelesions(2). With the clinical progression,lesions tend to decrease in size, calcify, and increase itsechogenicity as a result of fibrosis(23).Small, more frequent infarction zones are hardly differentiatedfrom small tumors (which may be equally avascular), however thetriangular-shaped infarction is a discriminative semiologicalelement(2). Amongst the differential diagnosis, one should considertesticular tumor and abscess which present a diverse clinicalhistory(11). In dubious cases, magneticresonance imaging shows the gadolinium enhancement in tumorprocesses, and absent enhancement ininfarction(2). Hemorrhagic infarcts may rarely occur as a complication ofinguinal hernioplasty. The anatomopathological substrate is thevenous flow interruption, generating local congestion andhemorrhagic necrosis. At ultrasound, an increase in testis is observed with diffuseheterogeneity associated with permeated hyperechogenic areas,suggesting zones of liquefaction looking like a thick fluid. At magnetic resonance imaging, T1-weighted sequencesdemonstrate an increased signal typical of hemorrhagiccollections, because of products from hemoglobindegradation(2).
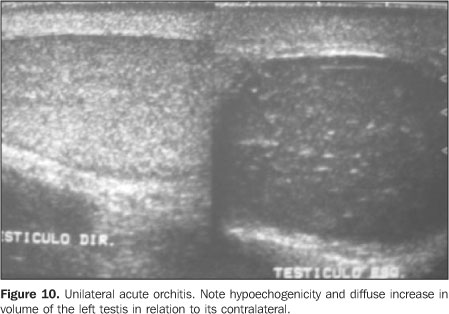
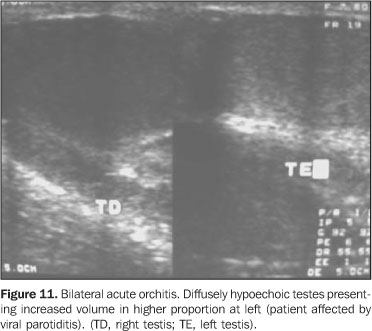
ACUTE ORCHITIS Usually orchitis results from a direct extension of epididymisinflammation to testis, which becomes acutely edematous andpainful(1,23). Primary orchitis is frequentlyviral and associated with parotiditis. Contrarily to bacterialorchiepididymitis, the viral infections usually arebilateral(1). In adolescents, most common causing agents are those sexuallytransmitted like Chlamydia trachomatis and Neisseriagonorrhoeae. In prepubertal boys and men aged above 35 years,most frequently the disease is caused by Escherichia coliand Proteus mirabilis(24). Ultrasound shows indirect signs of inflammation such as hydrocele or pyocele associated with scrotal wall thickening, these forms being present in most of cases. The diffuse testicular involvement is confirmed by increase in parenchymal volume as a result of testicular edema, presenting a heterogeneous echotexture(21). In focal processes, presentation is characterized by multiple hypoechoic lesions scattered throughout the parenchyma(21) (Figure 10). In viral orchitis there is a diffuse increase in volume, and homogeneous or heterogeneous hypoechogenicity with peripheral hypoechoic zones(1) (Figure 11).
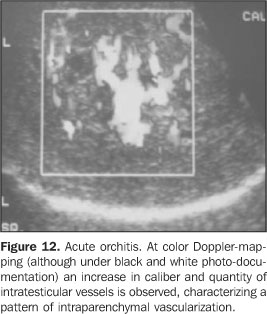
Since these findings are not specific of orchitis, they mustbe correlated with clinical history and laboratory tests. Thepatient should be followed-up until complete resolution.Additionally, findings must be documented by ultrasound aiming atruling out tumor, infarction and metastasis. At color Doppler-mapping, one observes an increase in the blood flow into epididymis and testis, characterized by increased number of vascular structures identifiable per view field which must always be compared with the contralateral testis. The analysis of the resistivity index and spectral pattern may bring useful information, since in these cases there is a decrease in the vascular resistance in relation to healthy individuals(25) (Figure 12).
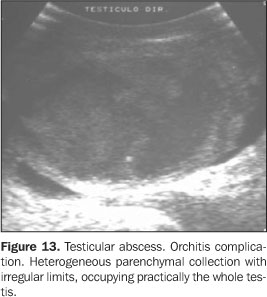
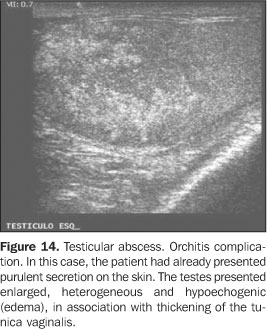
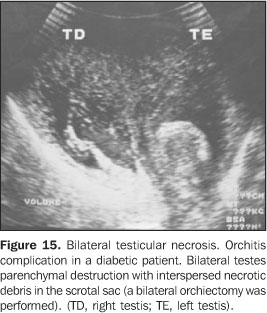
In this context, ultrasound also becomes essential forresearching the process severity, the complications, and elementsof differential diagnosis like a subacute testiculartorsion(1). A relatively frequent infectious complication is the abscess,corresponding to a hypoechogenic fluid collection with poorlydefined contours and a hypo/hyperechogenic halo, sometimesassociated with echogenic débris. The color Doppler-mapping shows an increase in the perilesional vascularization and absent blood flow inside the abscess. Rarely, gas bubbles can be observed, appearing like hyperechoic, supernatant punctate foci(1) (Figures13, 14 and 15).
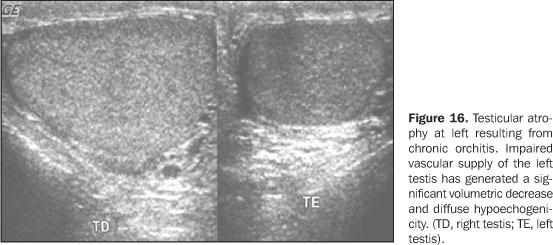
Another complication is the acute ischemia generated by compression of the vascular pedicle of the spermatic cord with the resulting formation of intratesticular venous thrombi. At the color Doppler-mapping, decreased or absent vascularization is observed, in contrast to the adjacent epididymis hypervascularization(1). With the clinical progression, the affected testis atrophy is observed (Figure 16).
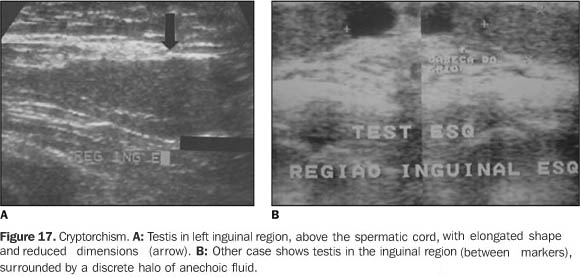
CRYPTORCHISM AND ECTOPIA The frequency of cryptorchism in the population ranges between0.5% and 0.8%. The undescended testis may be situated from therenal hilus to the inguinal canal. In one-third of cases isbilateral, but in cases of unilaterality the right side is mostfrequently affected. Most common localization is in the inguinalcanal (72% of cases), followed by the prescrotal (20%) andabdominal or pelvic topography (8%)(1). Testicular ectopia is a quite rare condition, and the mostfrequent localization is the subcutaneous region situated betweenthe internal and external inguinalfossas(21). All cases of cryptorchism must be surgically treated(orchidopexy or rudimentary testis ablation) to avoid futurecomplications such as infertility, tumor process, torsion andincarceration of intestinal loops. The risk for malignantdegeneration is 48 times superior to that in the normal testis,seminoma and embryonic carcinoma being the most frequent types oftumors(1). At ultrasound, the cryptorchidic testis appears atrophic, hypoechoic, homogeneous or heterogeneous (Figure 17). In its most frequent localization, the external inguinal canal opening is identifiable by echography. In the cases where this opening is localized in the deep opening of the inguinal canal, the presence of gas reverberation artifacts from the digestive apparatus complicate the visualization of a small testis; so in these cases magnetic resonance imaging is the indicated modality(1).
RARE TESTICULAR DISEASES Ectopic rests of adrenal tissue During the embryonal development, some adrenocortical cellsmay remain in the testicular parenchyma, and, unless they receivesufficient hormonal stimulation, remain undetectable. In childrenwith congenital adrenal hyperplasia, there is a defect in theglucocorticoid synthesis and possible intratesticular adrenalrests are abnormally stimulates, suffering from hypertrophy. Thelesions tend to be detected by ultrasound as multiple,round-shaped and hypoechoic(6,16). Theselesions are not considered as potentiallymalignant(23). Sarcoidosis Sarcoidosis rarely affects the testis, with genitalinvolvement occurring in only 1% of patients with systemicinvolvement. Usually, it causes a painless enlargement of thetestis, and at ultrasound irregular, solid, hypoechoic andpotentially calcifying lesions areidentified(2,23). Tuberculosis and syphilis may present similar sonographicmanifestations, and should be considered as differentialdiagnosis(23). When this disease presents witha focal pattern, the differential diagnosis with other tumor-likelesions is not feasible with ultrasound(2). Splenogonadal fusion The testicular fusion with splenic tissue is an unusualfinding, and may be discontinuous (intratesticular ectopicsplenic tissue), or continuous (direct connection between thespleen and gonad by a fibrous cord)(26).Clinically, the patients present with an inguinal or scrotalmass; lesions larger than 5 cm have already been described.Frequent associated findings are: hernia, cryptorchism andmicrognathia(16). Intratesticular arteriovenous malformation An intratesticular arteriovenous malformation is a rareentity, and the differential diagnosis is hemangioma. Thiscondition usually presents like a hypoechoic nodule, and at colorDoppler demonstrates a blood flow pattern with low impedance,high diastolic peak velocity, and presence of a drainagevein(27).
REFERENCES 1. Roy C, Tuchmann C. Échografie scrotale – pathologies non tumorales courantes (part 1). J Radiol 2003;84:581–595. [ ] 2. Roy C, Tuchmann C. Échografie scrotale – pathologies kystiques, tumorales et non tumorales rares (part 2). J Radiol 2003;84:667–680. [ ] 3. Hobarth K, Susani M, Szabo N, Kratzik C. Incidence of testicular microlithiasis. Urology 1992; 40:464–467. [ ] 4. Cast JEI, Nelson WM, Early AS, et al. Testicular microlithiasis: prevalence and tumor risk in a population referred for scrotal sonography. AJR Am J Roentgenol 2000;175:1703–1706 [ ] 5. Backus ML, Mack LA, Middleton WD, King BF, Winter TC III, True LD. Testicular microlithiasis imaging appearances and pathologic correlation. Radiology 1994;192:781–785. [ ] 6. Dambro TJ, Stewart RR, Barbara CA. The scrotum. In: Rumack CM, Wilson SR, Charboneau JW, editors. Diagnostic ultrasound. 2nd ed. St Louis: Mosby, 1998;791–821. [ ] 7. Frush DP, Kliewer MA, Madden JF. Testicular microlithiasis and subsequent development of metastatic germ cell tumor. AJR Am J Roentgenol 1996;167:889–890. [ ] 8. Diego AC, Rasines GL, Rodriguez RH. Lesiones testiculares que no hay que tocar. Arch Esp Urol 2003;56:255–266. [ ] 9. Janzen DL, Mathieson JR, Marsh JI, et al. Testicular microlithiasis: sonographic and clinical features. AJR Am J Roentgenol 1992;158:1057–1060. [ ] 10. Abbehusen C, Oliveira JMA, Granero L, Ajzen AS, Szejnfeld J. O valor do ultrassom na microlitíase testicular. Urologia on line 1998;2(5):sp. [citado agosto 2004]. Disponível em: http://www. unifesp.br/dcir/urologia/uronline [ ] 11. Dogra VS, Gottlieb RH, Rubens DF, Liao L. Benign intratesticular cystic lesions: US features. RadioGraphics 2001;21 Spec No:S273–S281. [ ] 12. Rifkin MD, Jacobs JA. Simple testicular cyst diagnosed preoperatively by ultrasound. J Urol 1983;129:982–983. [ ] 13. Rezende DEL. Cisto simples de testículo: relato de caso e revisão da literatura. Radiol Bras 2001; 34:251–252. [ ] 14. Yalowitz BR, Eble JN, Wilks DC. Spermatozoa-containing simple cysts of the rete testis. J Urol 1989;142:1572–1573. [ ] 15. Davis RS. Intratesticular spermatocele. Urology 1998;51(SA Suppl):167–169. [ ] 16. Rubenstein RA, Dogra VS, Seftel AD, Renick MI. Benign intrascrotal lesions. J Urol 2004;171: 1765–1772. [ ] 17. Das KM, Prasad K, Szmigielski W, Noorani N. Intratesticular varicocele: evaluation using conventional and Doppler sonography. AJR Am J Roentgenol 1999;173:1079–1083. [ ] 18. O'Donell PG, Dewbury KC. The ultrasound appearances of intratesticular varicocele. Br J Radiol 1998;71:324–325. [ ] 19. Atasoy C, Fitoz S. Gray-scale and color Doppler sonographic findings in intratesticular varicocele. J Clin Ultrasound 2001;29:369–373. [ ] 20. Burrus JK, Lockhart ME, Kenney PJ, Kolettis PN. Cystic ectasia of the rete testis: clinical and radiographic features. J Urol 2002;168(4 Pt 1):1436–1438. [ ] 21. Dogra VS, Gottlieb RH, Oka M, Rubens DJ. Sonography of the scrotum. Radiology 2003;227: 18–36. [ ] 22. Rouviere O, Bouvier R, Pangaud C, Jeune C, Dawahra M, Lyonnet D. Tubular ectasia of the rete testis: a potential pitfall in scrotal imaging. Eur Radiol 1999;9:1862–1868. [ ] 23. Howlett DC, Marchbank NDP, Sallomi DF. Pictorial review. Ultrasound of the testis. Clin Radiol 2000;55:595–601. [ ] 24. Luker GD, Siegel MJ. Color Doppler sonography of the scrotum in children. AJR Am J Roentgenol 1994;163:649–655. [ ] 25. Middleton WD, Siegel BA, Melson GL, Yates CK, Andriole GL. Acute scrotal disorders: prospective comparison of color Doppler US and testicular scintigraphy. Radiology 1990;177:177–181. [ ] 26. Putschar WG, Manion WC. Splenic-gonadal fusion. Am J Pathol 1956;32:15–33. [ ] 27. Kutlu R, Alkan A, Soylu A, Sigirci A, Dusak A. Intratesticular arteriovenous malformation: color Doppler sonographis findings. J Ultrasound Med 2003;22:295–298. [ ]
Received October 28, 2004.
* Study developed at Department of Diagnostic Imaging – Universidade Federal de São Paulo/Escola Paulista de Medicina, São Paulo, SP, Brazil. |
|
Av. Paulista, 37 - 7° andar - Conj. 71 - CEP 01311-902 - São Paulo - SP - Brazil - Phone: (11) 3372-4544 - Fax: (11) 3372-4554