Radiologia Brasileira - Publicação Científica Oficial do Colégio Brasileiro de Radiologia
AMB - Associação Médica Brasileira CNA - Comissão Nacional de Acreditação
 Vol. 42 nº 1 - Jan. /Feb. of 2009
Vol. 42 nº 1 - Jan. /Feb. of 2009
|
ICONOGRAPHIC ESSAY
|
|
Congenital mediastinal cysts: imaging findings |
|
|
Autho(rs): Tiago Tavares Vilela, Renato Tavares Daher, Mariana Domiciano Albuquerque Nóbrega, Carlos Alberto Ximenes Filho, Cristiano Montandon, Marcelo Eustáquio Montandon Júnior |
|
|
Keywords: Congenital mediastinal cysts, Cystic neoplasms, Cysts |
|
|
Abstract:
IMD, Radiologist, Trainee at Unit of Magnetic Resonance Imaging, Department of Radiology and Imaging Diagnosis - Santa Casa de Misericórdia de São Paulo, São Paulo, SP, Brazil
INTRODUCTION Congenital mediastinal cysts are benign lesions caused by abnormal embryological development of the anterior intestine and/or coelomic cavity(1). These lesions represent 10% of the mediastinal masses and include, among their main entities, bronchogenic, pericardial, enteric, thymic, esophageal duplication cysts and lymphangiomas, generally asymptomatic although sometimes may present as a medical emergency, particularly because of adjacent organs compression. Imaging methods, especially computed tomography (CT) capable of evaluating the density of such structures, play a critical role in the diagnostic elucidation and therapy planning if necessary. Other parameters such as localization and change in the lesional aspect according to the different patient positionings (for example, decubitus and orthostatic position) also can be relevant in the differential diagnosis, especially in the interpretation of radiographic images of the chest. Therefore, radiologist's familiarity with this theme is crucial, considering that most of times, their reports are the ending point of the diagnostic investigation. Ten cases were selected from the records of the institution where the present study was developed in the period between 1999 and 2006, and six of these cases were confirmed by surgical and histopathological findings. The diagnoses of the other four cases were based on imaging findings and on the progression along the follow-up. Among the cases included in this study, three pericardial cysts, three bronchogenic cysts, one esophageal duplication cyst, one enteric cyst, one thymic cyst, and one lymphangioma were diagnosed. No prevalence of these lesions in male or female individuals was observed, and the mean patients' age at the moment of the diagnosis was 40 years, ranging from 5 to 70 years.
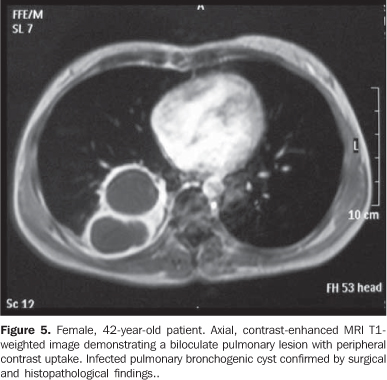
DISCUSSION At CT, congenital mediastinal cysts are characterized as expansile, internally hypodense and homogeneous lesions with well-defined thin walls. Although these lesions are generally Noncontrast uptaking (Figure 1), capsular enhancement may be observed in a minority of cases and also in the evaluation by magnetic resonance imaging (MRI)(2). The initial evaluation by chest radiography is a useful diagnostic tool, demonstrating a radiodense, expansile lesion with variable localization whose aspect can change according to the different patient positionings (for example, dorsal decubitus and orthostatic position). Because of the absence o ionizing radiation, ultrasono-graphy (US) is more appropriate for the pediatric group, generally demonstrating an anechoic, homogeneous, well-defined cystic lesion confined either to a single or multiple mediastinal compartments. Clinical manifestations, when present, result principally from extrinsic compression of adjacent structures such as the tracheobronchial tree (dyspnea, stridor) and esophagus (dysphagia). Other possible presentations result from rupture, infection (see Figure 5), and hemorrhage(3,4). In the case of hemorrhage, CT demonstrates an increase in size and density of the cyst, complicating the differential diagnosis with solid lesions(2). So, it is essential that the mass density is measured before and after intravenous contrast injection, since a density of > 10 Hounsfield units is considered as significant, indicating the presence of a solid lesion.
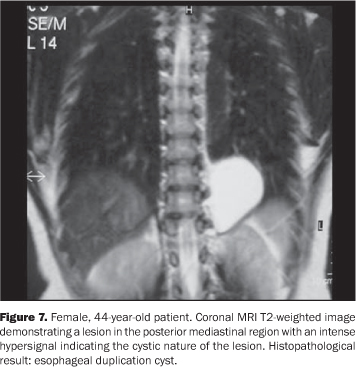
MRI can also be useful in this differentiation of cystic lesions because of the high signal intensity observed on T2-weighted sequences (see Figure 7). Among the mentioned methods, CT stands out by the high sensitivity and relative availability.
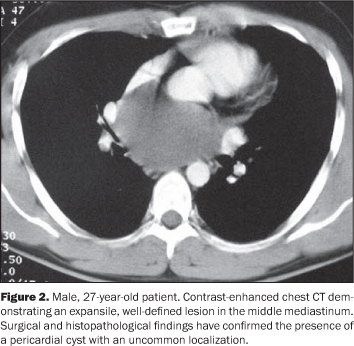
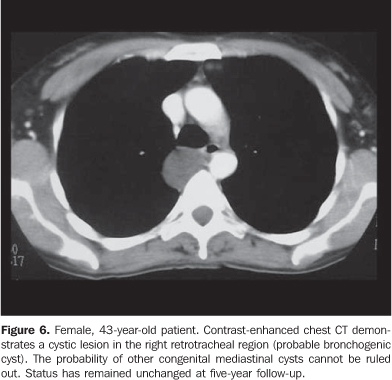
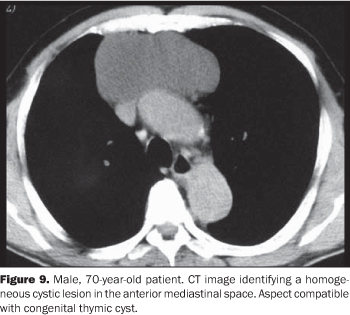
The proper determination of the specific nature of the different types of congenital mediastinal cystic masses is not always feasible, and in this case these lesions are otherwise classified as foregut cysts. In the present paper, the main types of congenital mediastinal cystic lesions are separately described. Pericardial cysts Pericardial cysts results from anomalies in the formation of coelomic cavities. These lesions are invariably attached to the pericardial leaflet, although communication with the pericardial cavity is observed in only few cases(1). Classically, pericardial cysts arise adjacent to the right anterior cardio-phrenic angle, but less frequently can also be seen at other sites such as the superior pericardial recess(5) (Figure 2). Occasionally, the cysts may demonstrate rectilinear contour and atypical shapes (for example, triangular), probably because of parietal adhesion. Among the pericardial cysts described in the present study two were found in the middle mediastinum and one in the anterior mediastinum. Figure 3 is an example of the classical CT imaging finding of this entity, demonstrating an expansile, hypo-dense lesion adjacent to the right anterior cardiophrenic angle. The blurring of the cardiac silhouette on the postero-anterior chest radiograph indicates the anterior positioning of this lesion (silhouette signal). Bronchogenic cysts Bronchogenic cysts originate from abnormal foregut protrusion in the period between the 26th and 40th days of pregnancy(1). From the histopathological point of view, these lesions are lined with a ciliated columnar epithelium with a cartilaginous component and, less frequently, bronchial glands. Most frequently, these lesions are found in the middle mediastinum, near the tracheal carina, and less frequently in any part of the mediastinum and chest such as lungs, pleura and diaphragm(3,6). Parietal calcifications can occasionally be observed (Figure 4). The present casuistic is in contrast to the classical description of this entity, demonstrating one case with intrapulmonary localization (Figure 5) and the other two in the upper mediastinal region (right para-tracheal and retrotracheal - respectively Figures 5 and 6). Esophageal duplication cyst Esophageal duplication cysts are classified into three groups according to their histopathological characteristics(1): in the first group, a lesion adjacent to the esophageal wall is observed; the second group comprises the rarest presentation characterized by an extrinsic lesion communicating with the esophageal body; and the third group includes intramural, extramucosal lesions. These lesions are most frequently found in the posterior mediastinum, near the thoracoabdominal transition (Figure 7). Occasionally, gastric mucosa may be observed within these lesions, resulting in peptic complications such as ulcer and perforation(7,8). Enteric cysts Enteric cysts are uncommon lesions, typically localized in the posterior mediastinum without a communication with the esophagus. The association of these lesions with vertebral abnormalities, particularly hemivertebra, is well documented(1). Presence of gastric mucosa with the possible complications may also be observed. Figure 8 represents the classical description of these lesions, with posterior mediastinal localization and association with hemi-vertebra. Thymic cysts Thymic cysts represent 3% of anterior mediastinal lesions and can be congenital or acquired. The first group are similar to the other congenital mediastinal cysts, with regular contour and homogeneous and hypodense contents. Acquired lesions are frequently associated with inflammatory/infectious processes (HIV, lupus and Sjögren's disease, among others) and neoplastic processes (such as non-Hodgkin lymphoma and, less frequently, thymoma, thymic carcinoma and mediastinal seminoma) presenting like heterogeneous, multilocular formations with intermingled septations. The differentiation between congenital and acquired lesions is important, considering that acquired lesions require histopathological study to rule out the association with neoplasms(9). In these cases, the utilization of intravenous contrast agent is essential for demonstrating intralesional septations in acquired thymic cysts otherwise indistinguishable on non-contrast enhanced studies(10). The present study demonstrates an anterior mediastinal well-defined, homogeneous, hypodense lesion compatible with congenital thymic cyst in an asymptomatic elder patient (Figure 9).
Lymphangiomas Lymphangiomas are congenital benign lesions characterized by focal proliferation of lymphatic tissue with a multicystic pattern. These lesions are histologically classified according to the depth and size of lymphatic vessels involved, as follows: simple (capillary), cavernous and cystic (hygroma), this later being the most frequently found(1). Axillas and neck are most commonly affected. Primary thoracic lesions correspond to only 1% of cases(2). With a predominantly cystic composition, these lesions may present with septa and, less frequently, with a solid component. Calcifications are rarely observed. Generally, because of their soft consistency, these lesions tend to develop without compressing adjacent structures. The lymphangioma described in the present study (Figure 10) is characterized by a bulky, cystic, homogeneous lesion in the posterior mediastinum, involving the descending aorta and the esophagus, with no sign of significant compression of these structures. One-year follow-up demonstrated a marked involution of this lesion.
CONCLUSION Familiarity with the localization and with imaging findings of congenital mediastinal cysts is essential, considering that, most of times, the definite diagnosis is based on the interpretation of imaging studies to avoid unnecessary invasive procedures.
REFERENCES 1. Gilbert-Barness E. Potter's Pathology of the fetus and infant. 4th ed. St. Louis: Mosby-Year Book; 1997. [ ] 2. Jeung MY, Gasser B, Gangi A, et al. Imaging of the cystic masses of the mediastinum. Radio-graphics. 2002;22:79-93. [ ] 3. McAdams HP, Kirejczyk WM, Rosado-de-Christenson ML, et al. Bronchogenic cyst: imaging features with clinical and histopathologic correlation. Radiology. 2000;217:441-6. [ ] 4. Berrocal T, Torres I, Gutiérrez J, et al. Congenital anomalies of the upper gastrointestinal tract. Radiographics. 1999;19:855-72. [ ] 5. Wang ZJ, Reddy GP, Gotway MB, et al. CT and MR imaging of pericardial disease. Radiographics. 2003;23 Spec No:S167-80. [ ] 6. Yoon YC, Lee KS, Kim TS, et al. Intrapulmonary bronchogenic cyst: CT and pathologic findings in five adult patients. AJR Am J Roentgenol. 2002; 179:167-70. [ ] 7. Franquet T, Erasmus JJ, Giménez A, et al. The retrotracheal space: normal anatomic and pathologic appearances. Radiographics. 2002;22 Spec No:S231-46. [ ] 8. Macpherson RI. Gastroinstestinal tract duplications: clinical, pathologic, etiologic, and radiologic considerations. Radiographics. 1993;13: 1063-80. [ ] 9. Choi YW, McAdams HP, Jeon SC, et al. Idiopathic multilocular thymic cyst: CT features with clinical and histopathologic correlation. AJR Am J Roentgenol. 2001;177:881-5. [ ] 10. Avila NA, Mueller BU, Carrasquillo JA, et al. Multilocular thymic cysts: imaging features in children with human immunodeficiency virus infection. Radiology. 1996;201:130-4. [ ] Received April 4, 2008. * Study developed in the Department of Radiology and Imaging Diagnosis - Hospital das Clínicas da Universidade Federal de Goiás (UFG), and Clínicas da Imagem e Multimagem, Goiânia, GO, Brazil. |
|
Av. Paulista, 37 - 7° andar - Conj. 71 - CEP 01311-902 - São Paulo - SP - Brazil - Phone: (11) 3372-4544 - Fax: (11) 3372-4554